Taking some basic, consistent precautions can help protect you and your family and prevent spreading the disease.
This is the first of a series about COVID-19 preparation and regional updates. Check the Press daily for new information, tips, and ways our health care professionals are working to keep our community safe.
The news of COVID-19 is everywhere, but not all of it is accurate. It is important for everyone to know the basic information about the virus, what symptoms to look for, and how to prevent spreading it to others.
What is COVID-19?
COVID-19 is a respiratory illness from the coronavirus family that can spread from person to person. According to the Centers for Disease Control and Prevention (CDC), the virus is thought to spread in the following ways:
- Between people who are in close contact with one another (within about 6 feet and at least 10+ minutes).
- Through respiratory droplets produced when an infected person coughs or sneezes.
- By touching a surface or object that has the virus on it and then touching your own mouth, nose, or possibly eyes.
What are the symptoms of COVID-19?
Patients with COVID-19 have had mild to severe respiratory illness with symptoms of:
- Fever (greater than 100.4 degrees)
- Cough
- Shortness of breath
How can I help protect myself?
You can protect yourself and others by using simple everyday preventive actions.
- Avoid close contact with people who are sick.
- Avoid touching your eyes, nose, and mouth with unwashed hands.
- Wash your hands often with soap and water for at least 20 seconds. Use an alcohol-based hand sanitizer that contains at least 60 percent alcohol if soap and water are not available.
How can I prevent spreading illness to others?
- Stay home when you are sick. Avoid public areas and do your best to distance yourself from others. Remain in self-isolation until a full day after your last symptoms if possible.
- Cover your cough or sneeze with a tissue, then throw the tissue in the trash.
- Clean and disinfect frequently touched objects and surfaces.
- And again, wash your hands frequently.
Who is the highest risk?
Older adults (over age 60) and those of any age who have severe underlying medical conditions like heart or lung disease or diabetes seem to be at higher risk for developing more serious complications from COVID-19. If you fall in this population, or care for someone who falls in this population the CDC recommends consulting with your health care provider about additional steps you may be able to take to protect yourself.
What is considered a mass gathering?
Idaho public health experts recommend postponing or canceling mass gatherings and public events in any of the following situations:
- The event will draw audiences or participants from communities, states, or countries with confirmed community spread of COVID-19 disease. Your local public health district can assist you in making this determination.
- The event will be held indoors and bring together more than 250 individuals where social distancing of 6 feet or more is unlikely or not possible.
- The event’s primary audience includes or may expose high-risk populations, including adults over the age of 60 years and people with underlying chronic medical conditions like heart or lung disease or diabetes, regardless of the number of attendees.
Why did PHD make recommendations on mass gatherings?
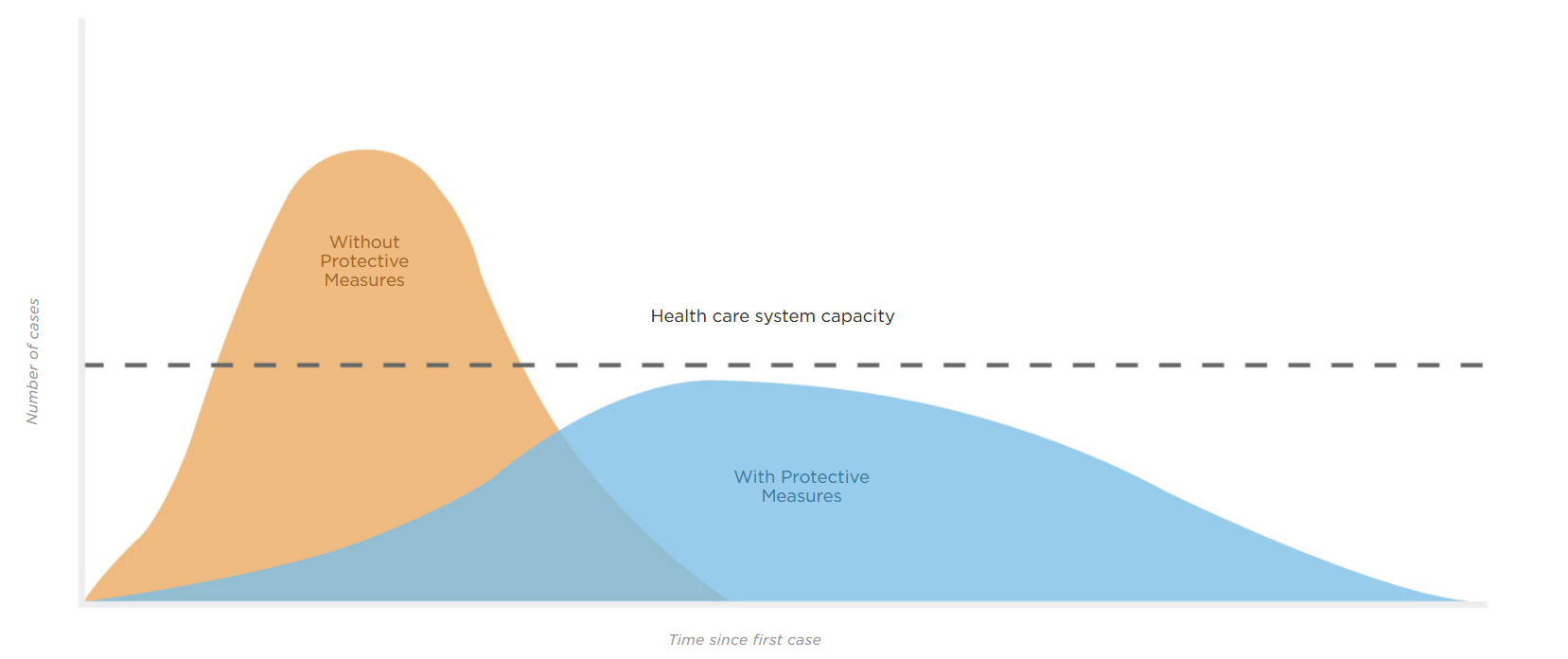
The Idaho Department of Health and Welfare and all seven of the health districts around the state developed guidance for mass gatherings and public events in order to protect our most vulnerable populations and slow the potential spread of the virus. Social distancing practices, like postponing events, is a proven effective tactic when mitigating the spread of a virus.
How can I be tested for COVID-19?
At this time, the Idaho Bureau of Laboratories is able to conduct testing and the CDC does confirmatory testing. PHD does not collect samples or test individuals. A person’s doctor will assess and arrange the collection of a sample if someone meets the criteria to be tested. The sample will be sent to the Idaho Bureau of Laboratories (IBL) to be tested. There is no fee for the sample to be tested by the IBL, but there will be provider fees.
Public health epidemiologists will prioritize testing. High priority will be given to specimens from symptomatic people who meet one or more of the following criteria:
- Had close contact with a person with a confirmed COVID-19 infection
- Recently traveled to an area with widespread community transmission of COVID-19 (China, Iran, Italy, South Korea)
- Have severe respiratory illness of no known cause
- Are health care workers
- Are long-term care facility residents with respiratory disease and negative influenza testing.
Can I be tested at a lab other than the State Lab?
Your provider can request a test based on his/her clinical judgment be done through a private lab, currently, the University of Washington’s Lab provides this testing and two commercial labs have announced their testing capability. LabCorp started testing for the novel coronavirus on March 6. ARUP Laboratories started testing on March 12. This information may change as more labs are available to conduct testing.
I’ve been tested for COVID-19, what now?
Until you receive your test results back, please stay home. This will reduce the spread of the virus if your test result is positive. If your symptoms progress to a level where you feel you need medical care, call your doctor or urgent care prior to going in. This will give medical professionals time to prepare and separate other patients and protect their staff.
Where can I find out the number of people being tested in Idaho?
The state of Idaho is posting updates on its site with the number of people being monitored and the number of people tested through the Idaho Bureau of Laboratories. You can find this information at coronavirus.idaho.gov.
While COVID-19 is making waves worldwide, in most cases it is manageable at home – much like the flu. You can find the information from this article as well as the latest updates and ways to protect yourself at cdc.gov/covid19.